What are the stages of CKD?
The progression of CKD varies for each individual and is influenced by factors like kidney function, underlying causes, and overall health. This article provides an informative overview of the stages of CKD, offering insights into the changes that occur as the disease advances.
The 5 Stages of CKD: Tracking Kidney Function and Damage
Chronic Kidney Disease (CKD) is a long-term condition in which the kidneys gradually lose their ability to function correctly, leading to a decline in kidney function and potential complications. The stages of CKD are defined based on the estimated Glomerular Filtration Rate (eGFR), which is a measure of kidney function, and the presence of kidney damage.
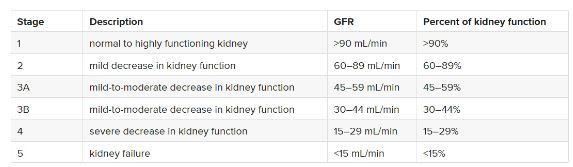
The 5 stages of CKD are as follows:
Stage 1: Kidney damage with normal or high eGFR
- eGFR > 90 mL/min/1.73 m²
- Kidney damage is present, but kidney function is still considered normal.
- Proteinuria (abnormal amounts of protein in the urine) may be detected.
- Usually, there are no symptoms in this stage.
Stage 2: Kidney damage with mild decrease in eGFR
- eGFR 60-89 mL/min/1.73 m²
- Kidney function is slightly impaired, but symptoms may still be absent. Fatigue
- itching, loss of appetite, sleep problems and weakness are initial and nonspecific symptoms.
- The kidneys are not working at full capacity, but the decreased function is mild.
Stage 3: Moderate decrease in eGFR
- eGFR 30-59 mL/min/1.73 m²
- Stage 3 is divided into two sub-stages:
- Stage 3a: eGFR 45-59 mL/min/1.73 m²
- Stage 3b: eGFR 30-44 mL/min/1.73 m²
- Kidney function is significantly reduced, and the following symptoms may start appearing:
- Back pain
- Fatigue
- Loss of appetite
- Constant itching
- Sleep problems
- Hands and feet might swell
- Too frequent or too rare urination
- Weakness
- Blood tests may show abnormalities related to kidney function.
- Complications associated with reduced kidney function may arise:
- Anaemia
- Bone disease
- High blood pressure
Stage 4: Severe decrease in eGFR
- eGFR 15-29 mL/min/1.73 m²
- Kidney function is markedly reduced.
- Symptoms and complications become more pronounced.
- While complications are the same as that in the case of stage 3 CKD, symptoms generally include:
- Back pain
- Chest pain
- Decreased mental sharpness
- Fatigue
- Loss of appetite
- Muscle twitches/cramps
- Nausea and vomiting
- Persistent itching
- Shortness of breath
- Sleep problems
- Hands and feet might swell
- Too frequent or too rare urination
- Weakness
- Preparation for kidney replacement therapy (dialysis or transplantation) often begins at this stage.
- At this stage the possibility of a heart disease or even a stroke increases.
Stage 5: End-stage kidney disease
- eGFR < 15 mL/min/1.73 m² or requiring dialysis
- This is the most advanced stage of CKD.
- Kidney function is severely impaired or completely lost.
- Symptoms that are usually severe and can affect overall health include:
- Back pain
- Chest pain
- Breathing problems
- Decreased mental sharpness
- Fatigue
- Little to zero appetite
- Muscle twitches/cramps
- Nausea or vomiting
- Persistent itching
- Trouble sleeping
- Severe weakness
- Hands and feet might swell
- Too frequent or too rare urination
- Dialysis or kidney transplantation is necessary to sustain life.
Watch this video to learn more about the five stages of chronic kidney disease in detail:
Managing and Treating Chronic Kidney Disease: Key Approaches for Optimal Care
Here are some key points about the treatment and management of CKD:
- Blood pressure control: Maintain optimal blood pressure levels through lifestyle changes and medication to slow CKD progression.
- Medications: Take prescribed medications to manage symptoms and complications like anaemia or mineral imbalances.
- Kidney-friendly diet: Follow a diet that controls protein, sodium, potassium, and phosphorus intake to lessen kidney burden.
- Fluid intake monitoring: Keep track of fluid intake to prevent fluid retention and complications.
- Regular monitoring and tests: Attend regular check-ups, blood, and urine tests to monitor kidney function and adjust treatment plans.
- Healthy lifestyle: Adopt a healthy lifestyle with regular exercise, weight management, no smoking, and limited alcohol intake slow CKD progression.
- Manage underlying conditions: Treat and manage underlying conditions contributing to CKD like hypertension or autoimmune disorders, to minimise kidney damage.
- Dialysis or transplantation: In advanced CKD stages, you must consider dialysis or kidney transplantation.
Conclusion
Remember, the progression of CKD can vary for each person, and proper management is crucial to slow down its progression and prevent complications. Regular monitoring and guidance from medical professionals are important for individuals with CKD.
FAQs
Q1. How long does it take to go from stage 3 to stage 4 kidney disease?
Ans. Most patients transition from stage 3 to stage 4 kidney disease in 10 years or above.
Q2. What foods are good for stage 5 CKD patients?
Ans. Fruits and vegetables contain less amount of potassium including grapes, green beans, cucumber, pasta, noodles and rice.